Learn Asbestosis: Diagrams



View Enlarged Diagram
Print Diagram
Anatomy of Frontal PA Chest X-Ray
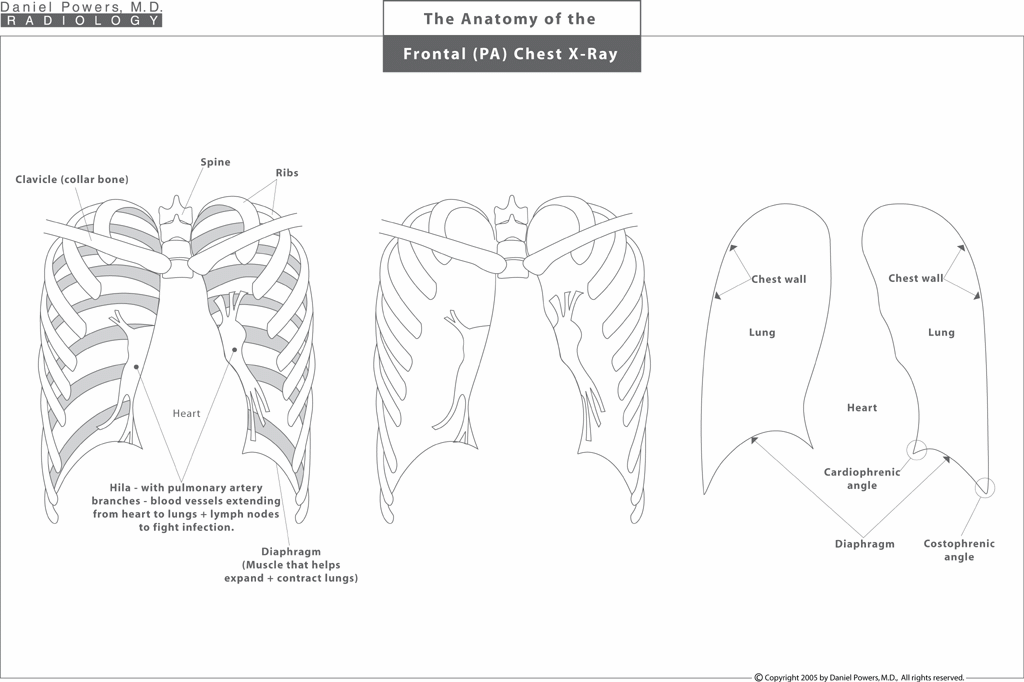
First, it is important that you understand the basic image that we are looking at. We are looking at a frontal view of the chest or the thoracic cavity, which consists of the heart in the middle, the spine in the back, the rib cage with the individual ribs forming an encasement surrounding the lungs, and the diaphragms at the bottom which, like bellows, helps the lungs expand and contract. The left-most image shows the anatomy of the thorax or chest and its cavity, which is gradually stripped down to give the right-most image, which is an outline of the anatomy of the chest that we need to understand - that is the heart in the center, the diaphragms or muscles that act like bellows at the bottom, the chest walls on the periphery and the lungs in between the heart and the chest walls.Frontal PA Chest X-Ray; Asbestos-Caused Pleural Changes
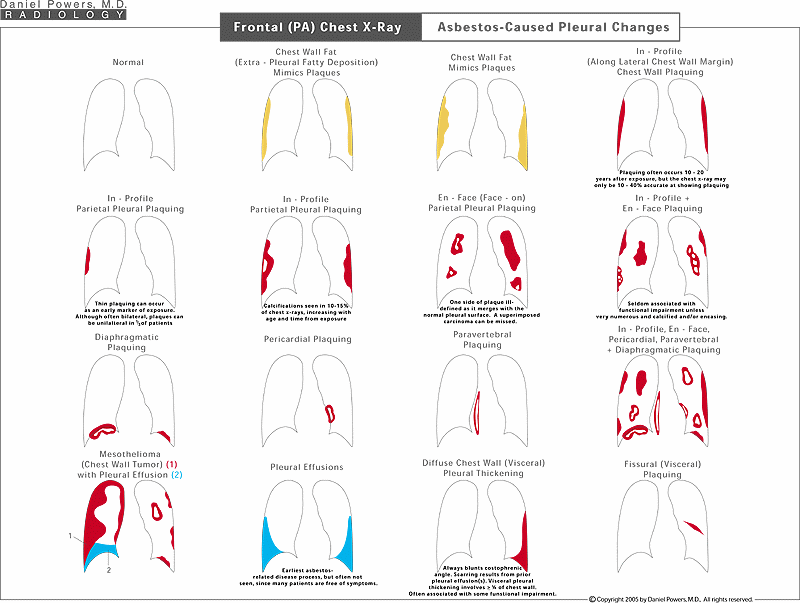
This visual diagram shows pleural changes that one would expect on plain radiographs. The far left image is a normal examination in which the chest wall is not thickened. Normal deposits of fat along the chest wall can cause thickening that mimics pleural plaquing. Pleural (circumscribed) plaquing can occur along the chest wall (parietal pleura) both on the side of the chest wall known as the "in profile" type, and face-on known as the "en face" type, along the front or back of the chest walls. Plaques can also occur on the linings overlying the diaphragms, the heart and the spine. Some of these plaques develop calcium deposits within them over time. In addition to pleural plaques, one can develop irritant fluid accumulations/"fluid-on-the-lung" known as pleural effusions, which are often temporary and frequently not known to the patient, since they may not cause pain or symptoms. However, after a pleural effusion, the lining of the lung (visceral pleura) can scar and thicken. This is known as diffuse pleural thickening. Often such visceral pleural thickening fuses with the lower chest wall parietal pleura resulting in blunting of the costophrenic angle. Visceral pleural thickening can occasionally occur between different lobes of the lung where the lining of the two lung lobes becomes irritated and subsequently fuse and thicken. Rarely, one can develop a cancer of the chest wall known as a mesothelioma, which is commonly associated with a malignant pleural effusion.Frontal (PA) Chest X-Ray; ILO Pleural Disease Classification
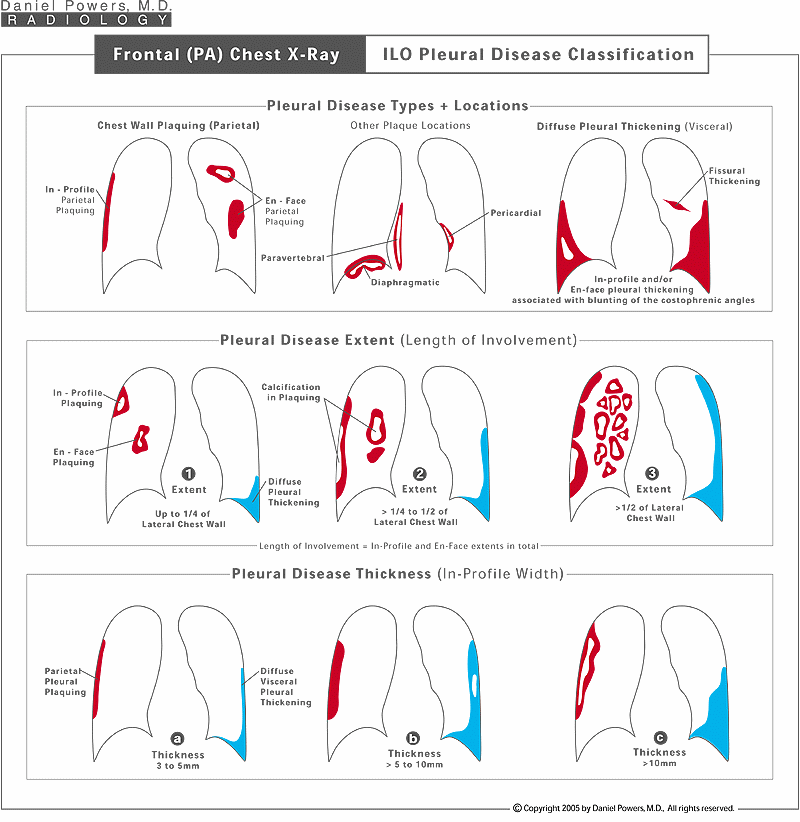
The ILO system classifies pleural (circumscribed) plaquing and diffuse pleural thickening. The pleural plaques can be "in profile" - along the side of the chest wall or "en face" being face-on, either along the front or the back walls of the chest cavity. They can also occur along the linings of the diaphragms, the spine, or adjacent to the heart. If there has been a pleural effusion, diffuse pleural thickening causing thickening of the lining of the lung, often with the lining of the lung sticking together with the lining of the chest wall can occur. The extent of the in profile and en face pleural plaquing is rated as "1", "2", or "3" - depending on whether it involves up to one-quarter of the lateral chest wall, greater than one-quarter up to one-half the lateral chest wall, or greater than one-half of the lateral chest wall. Similar classification occurs with diffuse pleural thickening. In addition, both the in profile pleural plaquing and in profile diffuse pleural thickening can be graded in terms of their thickness as "a" for 3 to 5 mm, "b" for greater than 5 to10 mm, and "c" for greater than 10 mm in thickness.Frontal (PA) Chest X-Ray; Pleural plus Pericardial Coverings
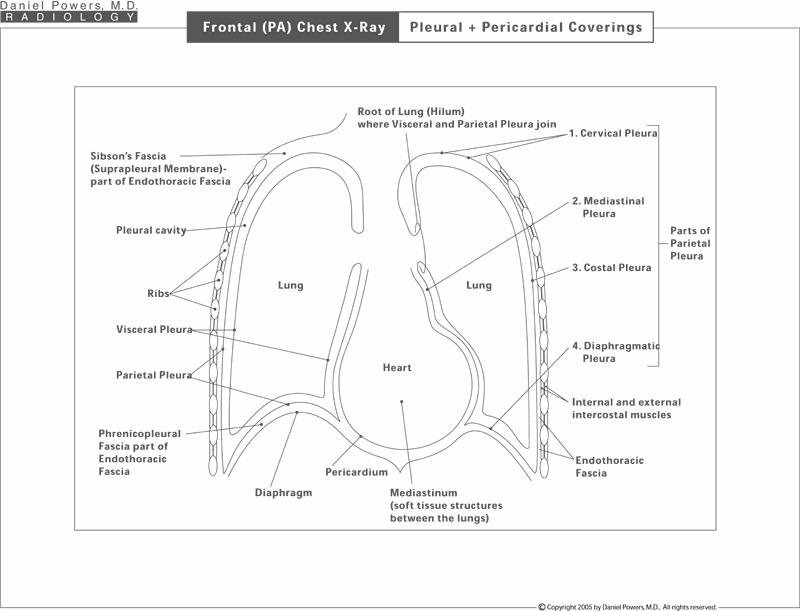
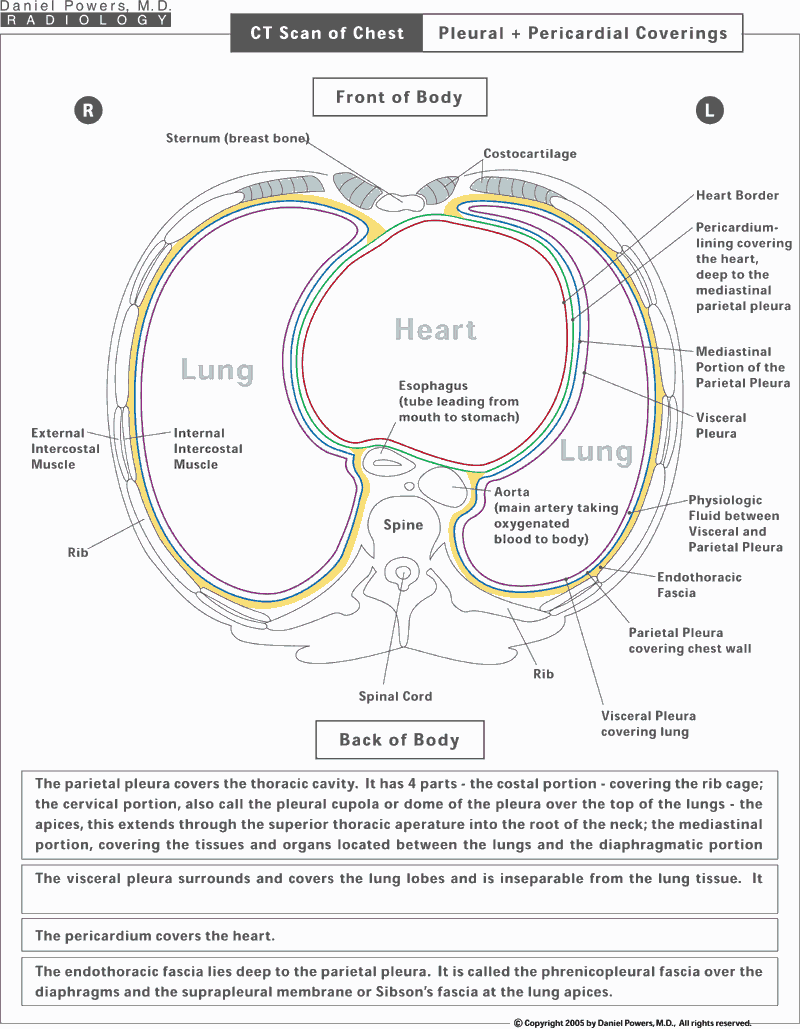
The chest cavity is composed primarily of the lungs on both sides with the heart in the middle, the spine in the back and the diaphragms on the bottom. The cavity itself is lined on the top, sides, bottom and in the mid-portion adjacent to the heart by a contiguous membrane, which has different names depending on the location. The parietal pleura - that portion of the lining that surrounds the chest cavity, but does not involve the lung itself, i.e., lines the rib cage, the diaphragms and the midline structures such as the heart. This is named the cervical pleura on the top, the mediastinal pleura in the middle, the costal pleura along the lateral chest walls, and the diaphragmatic pleura over the diaphragms. In addition, the lung itself is lined or covered by a membrane called the visceral pleura. The heart is also lined deep to the mediastinal pleura by another membrane known as the pericardium. Thus, a plaque along the margins of the heart is scarring to the mediastinal parietal pleura and not the pericardium or heart tissue below.CT Scan of Chest; Pleural plus Pericardial Coverings
Cross-sectional views of the thoracic cavity reveal the same information that needs to be known on the chest x-ray, but from a different perspective. The heart is surrounded by a membrane called the pericardium. This is in turn surrounded by a membrane called the mediastinal portion of the parietal pleura. The parietal pleura continues along the sides of the chest wall, where it is called the costal pleura, as well as superiorly over the top of the chest wall, known as the cervical pleura and along the bottom of the chest cavity over the diaphragms, known as the diaphragmatic pleura. The lung itself is also lined by a membrane known as the visceral pleura. Between the chest wall and the parietal pleural lining of it, is fat. This is where the fat deposits in some individuals mimicking pleural plaquing on chest x-ray. The fat is thus, extra-pleural (outside the pleura) and thus, the term extra-pleural fatty deposition is used to describe the location of this fat. It actually displaces the costal parietal pleura inward rather than representing thickening of the costal parietal pleura. The endothoracic fascia is located deep to the parietal pleura and it too has different names in different locations.Frontal (PA) Chest X-Ray; ILO Classification of the Amount of Lung Scarring: The Profusion
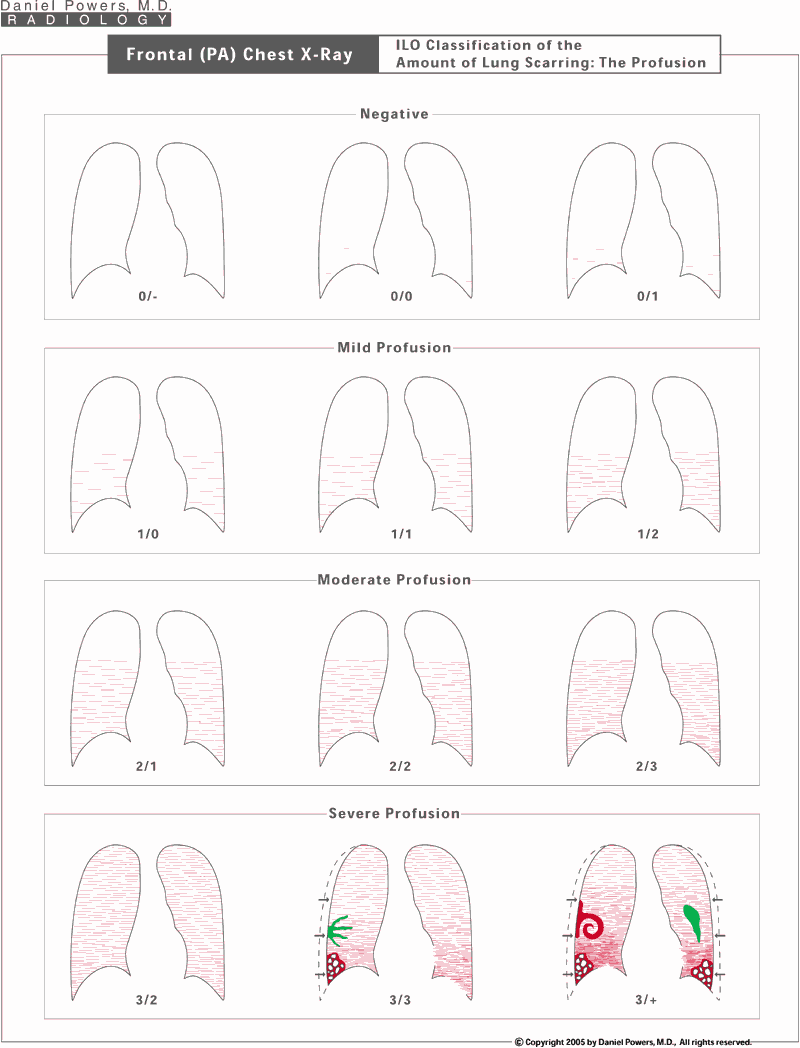
The International Labor Organization (ILO) grades scarring of the lung tissue (the interstitium or parenchyma) seen on the chest x-ray on a 12-point scale. Asbestos causes small irregular (and somewhat linear) opacities. The number of these irregular opacities per visual unit area is called the profusion, i.e., the intensity of the scarring or the amount of the visual snowstorm that is identified. The profusion is either considered anatomically insignificant/normal, which is given a grading of "0", of a mild amount given a grading of "1", of a moderate amount given a grading of "2", and of a severe amount given a grading of "3". Because doctors cannot always agree on the exact amount present, a fudge factor is added which basically allows for a minus or a plus in relationship to the number, such as an B-, B or B+ grade that a student might get in class. Thus, a 2/2 profusion represents a visually definite moderate amount of lung disease or visual profusion. A 2- would be a 2/1 meaning that the reader thinks that this chest x-ray is primarily of a moderate or 2-type profusion with a secondary thought that it is of a 1 or mild amount of profusion. A 2+ would be a 2/3, where the observer thinks that this is primarily of a moderate profusion, but is secondarily considering a severe profusion.Frontal (PA) Chest X-Ray; ILO Parenchymal Classifications
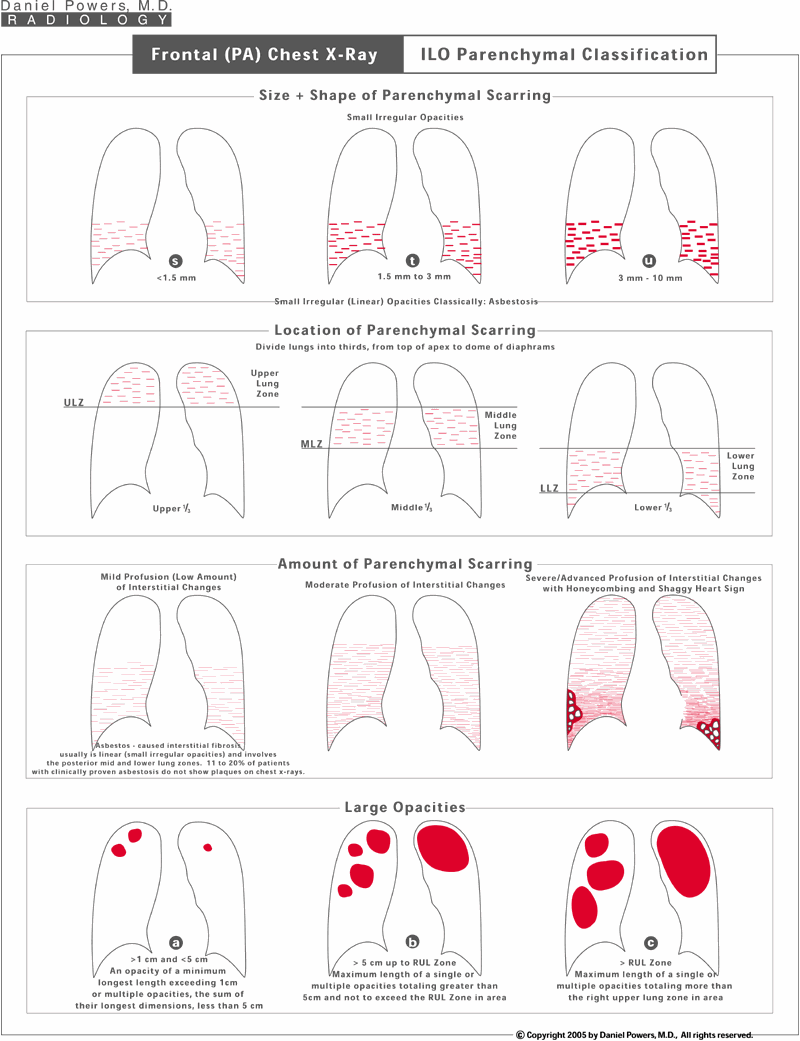
The lung scarring is also classified into the size and shape of the densities - being of an "s", "t" or "u" type for asbestosis; the location of the scarring - being upper, middle or lower lung zones; the amount of the scarring - mild, moderate or severe; and the presence or absence of larger conglomerate scars, known as "Large Opacities", which usually occur in diseases such as coal workers’ pneumoconiosis (black lung disease) or silicosis (sand blasters’ disease).Frontal (PA) Chest X-Ray ILO Symbols: 1 of 3
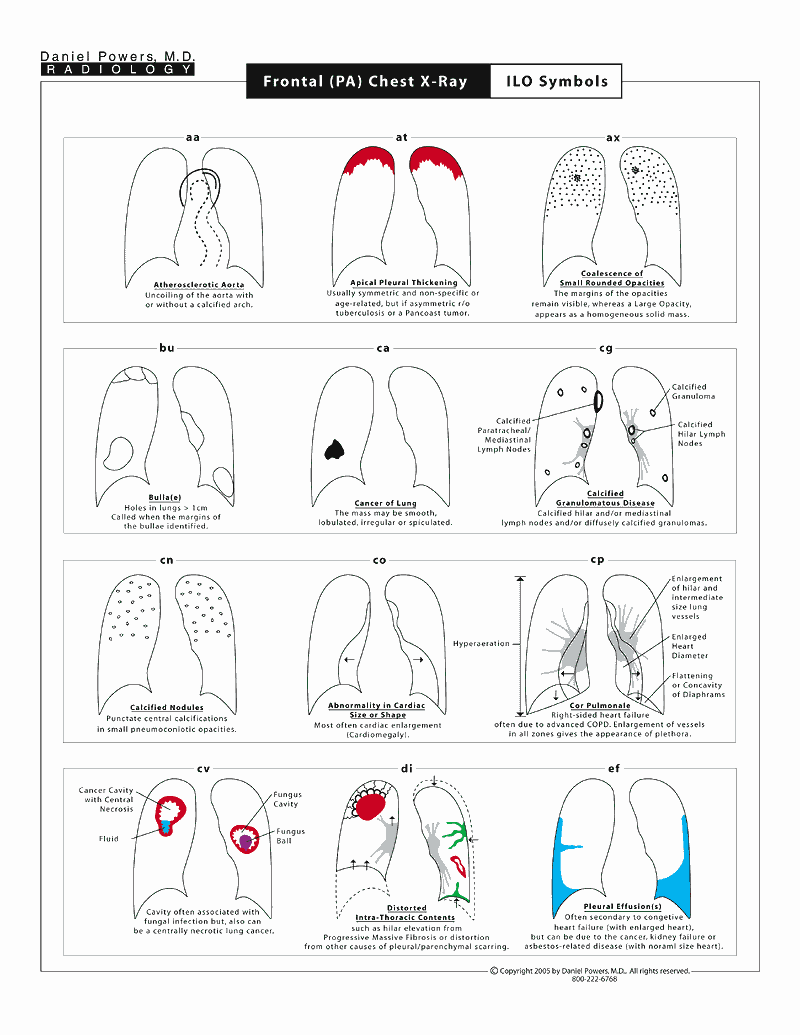
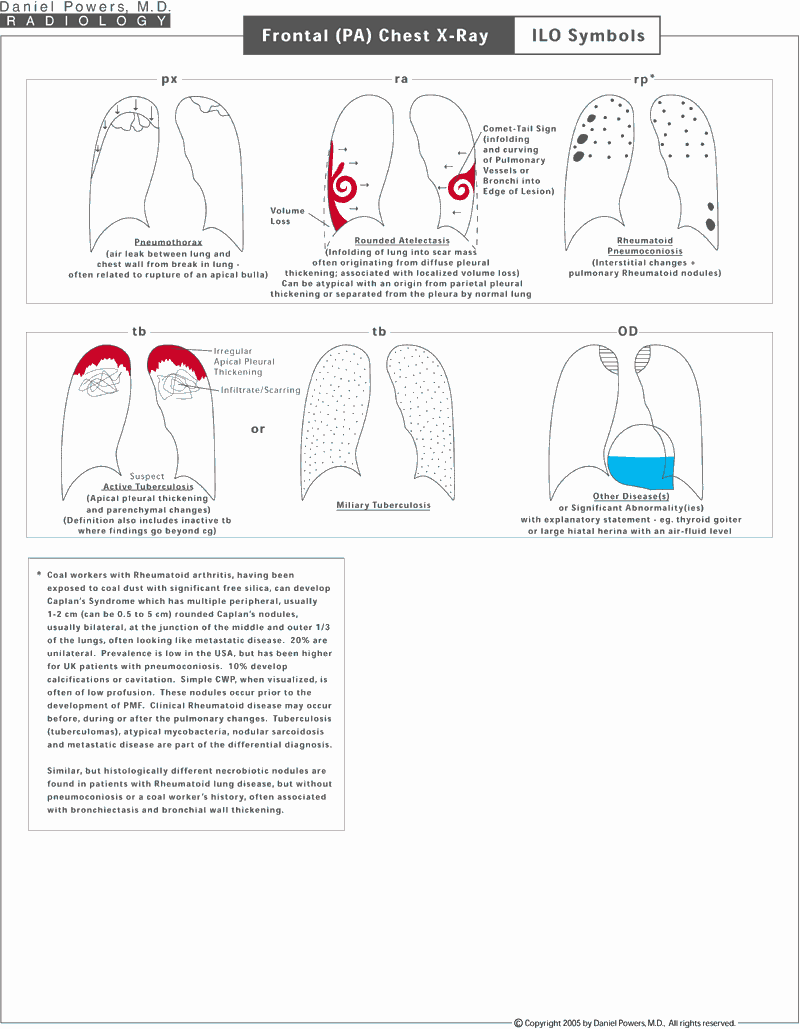
The following three pages describe the various symbols used on the ILO reporting form and visually shows what they would look like on chest x-rays.Supine Spiral CT Scan of the Chest; Chest Wall Views – Asbestos-Caused Findings
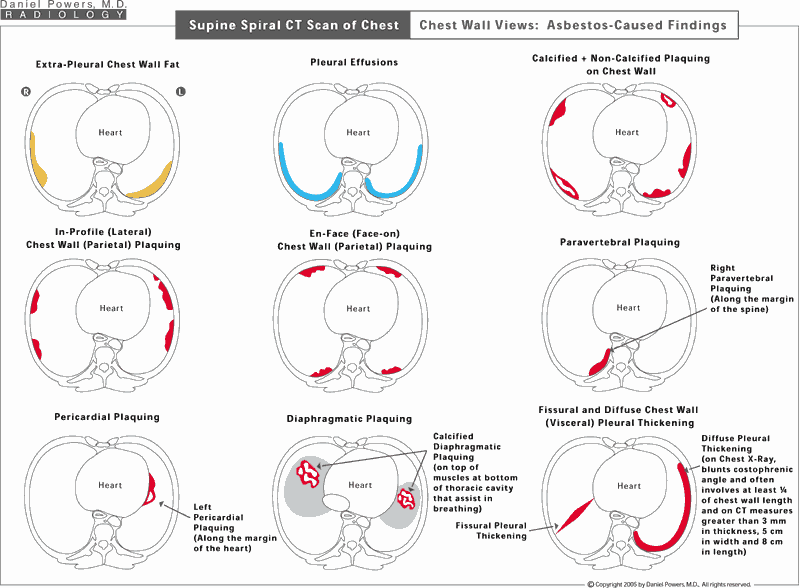
This diagram shows the findings that the Diagnostic Radiologist would identify on CT scans of the chest when the chest wall is thickened. Extra-pleural fat can mimic pleural plaques and is not caused by asbestos disease. CT is very helpful compared to chest x-rays since, on chest x-rays, one may not be able to tell the difference between an asbestos-caused pleural plaque and one that is due to normal variant fat, whereas on CT one can differentiate fat from plaques. CT is also helpful in identifying the presence or absence of a pleural effusion (fluid), which can be transient and may or may not be related to asbestos-caused problems depending on the patient’s clinical circumstances. For instance, if the patient were in heart failure, it is common to get fluid. However, in the proper clinical setting, in which a patient has an appropriate asbestos exposure history, a pleural effusion in the absence of other medical causes is probably secondary to an asbestos etiology. Pleural plaques are focal (circumscribed) areas of localized scarring adjacent to the chest wall, the heart, the spine, or the diaphragms (the parietal pleura) are described and seen. Diffuse pleural thickening (the visceral pleura) often occurs after pleural effusions and is also identified. Most of the time, it blunts the costophrenic angle on the involved side. CT is excellent at and better than the chest x-ray at showing calcifications in plaques. The presence of calcium in plaques is more definite proof of their presence, especially if they are thin and flat.Prone HRCT Scan of Chest Lung Parenchymal Views: Asbestos-Caused Findings
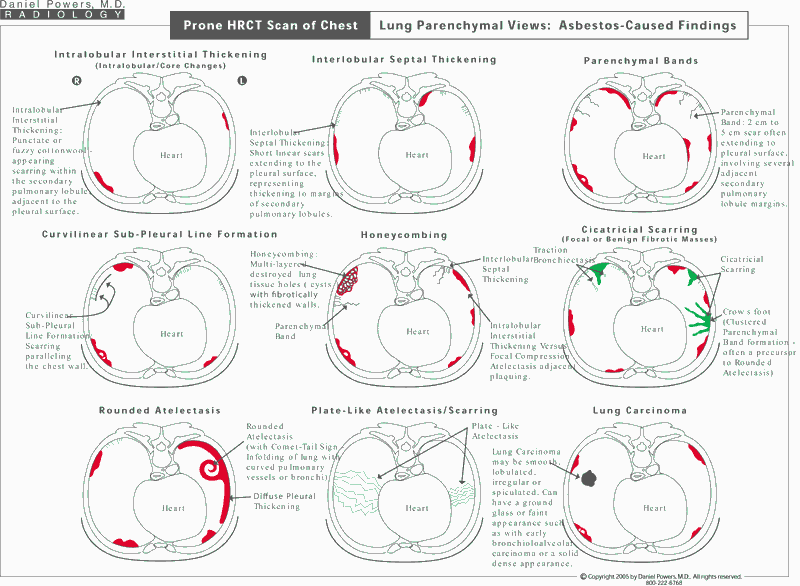
In asbestos disease, the majority of the lung parenchymal (tissue or interstitial) findings involve the mid and lower lung zones posteriorly. Because of this, it is best to obtain a prone study. The prone position removes the dependent atelectasis/gravitationally-caused localized collapse of the lung and blood pooling densities from the posterior aspects of the lung, which can mimic asbestosis. Asbestos-caused interstitial disease termed asbestosis can appear as intralobular interstitial thickening, interlobular septal thickening, non-dependent subpleural line formation, parenchymal bands and honeycombing. In addition, pleural changes can also be identified, including pleural effusion(s), (circumscribed, parietal) pleural plaquing, diffuse (visceral) pleural thickening, cicatricial masses and rounded atelectasis.
One may ask, why obtain both studies? The reason is that the supine spiral CT is a continuous scan from the top to the bottom of the lungs including the chest walls. It shows all of the areas without skips and is excellent for identifying the pleural changes as well as the presence or absence of a lung cancer. However, the slices are thick and there is often dependent density overlying the posterior aspects of the lung bases where asbestosis often appears. The prone HRCT is for lung parenchyma (tissue/interstitial) information, with thinner slices. The detail is much greater on HRCT (1 to 1.5 mm thick slices on prone HRCT versus 5 to 7 mm thick slices on supine spiral CT) and the prone position clears the posterior lungs of dependent atelectasis and blood pooling, to allow better visualization of lung parenchymal disease. To limit radiation exposure, the HRCT images are obtained at intervals - skipped areas result and thus, portions of the lungs and chest walls are not scanned. Small lung cancers or pleural plaques can be missed (located in the areas not scanned - in the skipped areas).Overcalling (Mimickers of) Disease AKA False Positives: Page 1 of 2
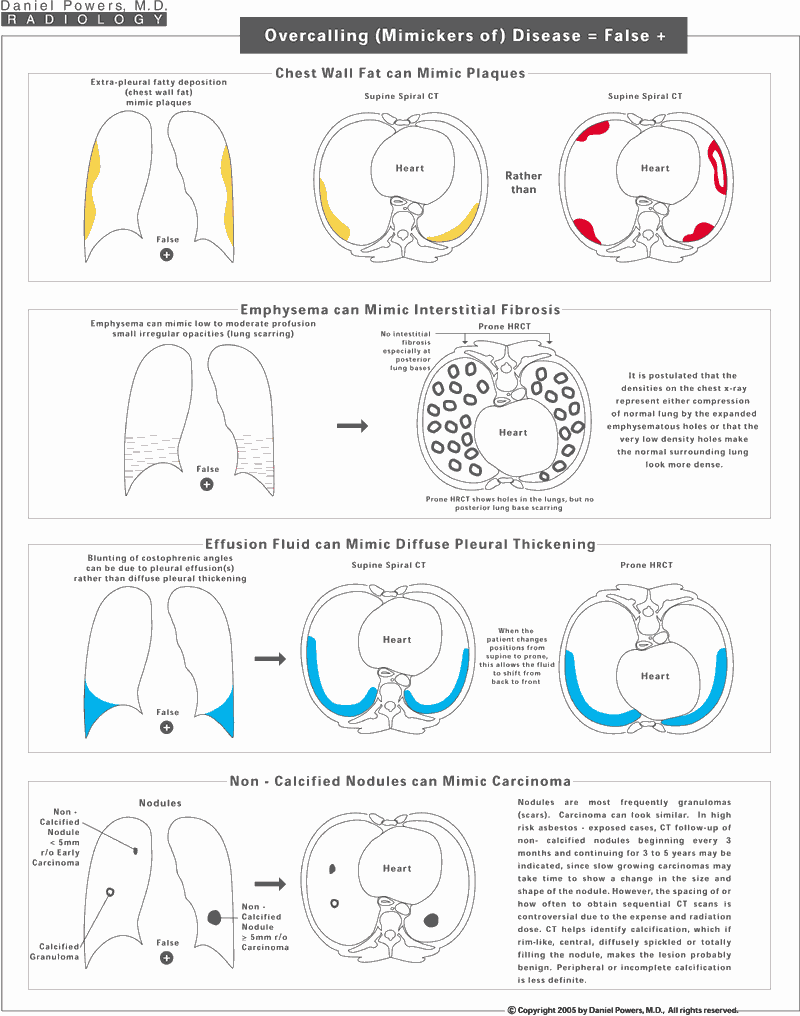
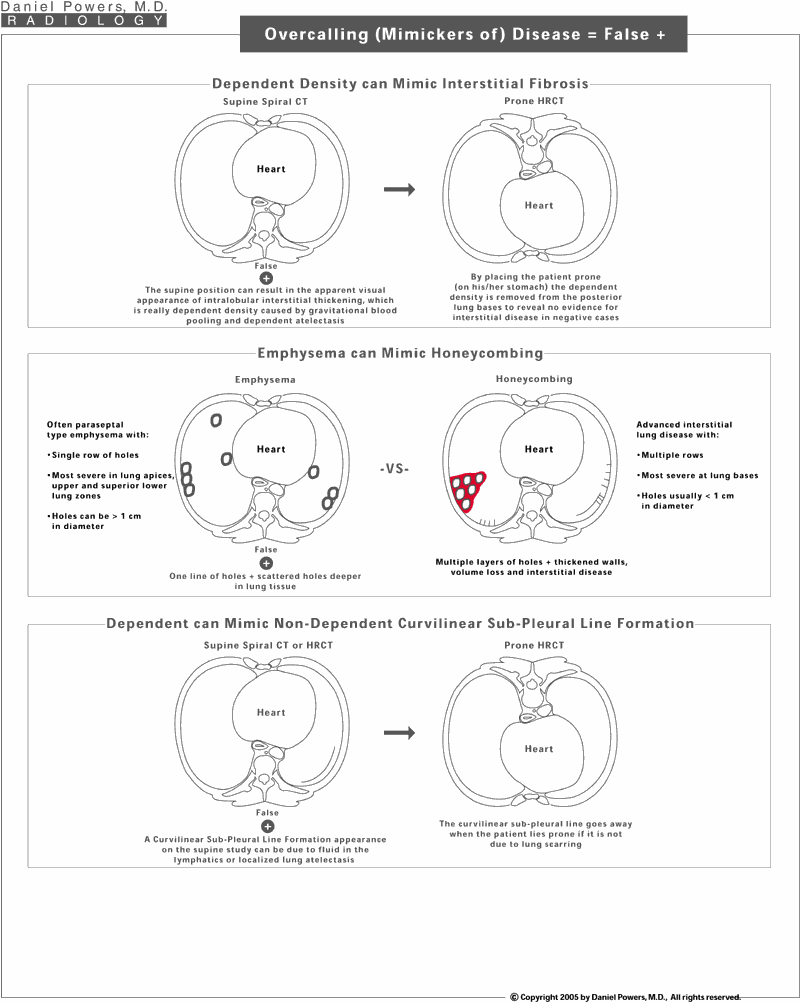
There are many findings that can appear like asbestos disease, when in fact, they are not. The skilled Diagnostic Radiologist or image reader is capable of separating these out especially when given the various types of imaging examinations simultaneously. Chest x-rays can have chest wall thickening due to fat rather than plaques. Chest x-rays can have densities within the lungs mimicking asbestosis, when in fact this is due to emphysema. Chest x-rays can show what appears to be diffuse pleural thickening, which may represent a transient pleural effusion. Non-calcified nodules can be common and be due to such things such as scars from prior infections known as granulomas rather than strictly representing a lung cancer or carcinoma. Depending on the size and appearance of the lesion, and the presence or absence of prior imaging studies, these masses/nodules/shadows often need sequential or follow-up imaging to determine whether they change in size or shape, i.e., whether they grow over time. Often a non-calcified appearing mass on chest x-ray can be evaluated by thin slice HRCT over the nodule to reveal calcium within it to justify it as being resulting from a prior benign scar. However, non-calcified nodules can be slow-growing cancers and as such, an unknown nodule in a high-risk patient needs to be followed for 3 to 5 years to exclude a slow-growing cancer.Overcalling (Mimickers of) Disease AKA False Positives: Page 2 of 2
Dependent gravitational pressure can cause localized collapse the posterior-most aspect of the lung, called dependent atelectasis or results in dependent gravitational accumulation of blood, known as blood pooling. Both cause a dependent ill-defined haze or density, which is commonly seen on the supine spiral or supine HRCT, along the back or posterior aspects of the lungs, adjacent to the posterior chest wall. By placing the patient prone (on one’s stomach), if this represents gravitationally dependent atelectasis and/or blood pooling, it shifts anteriorly and the posterior lung bases clear, if free of visible disease. Emphysema and honeycombing can be confused. Paraseptal emphysema tends to be single row of localized holes in the lung adjacent to the chest walls, heart, or fissures and will often commonly be in the upper lung zones as well. Honeycombing, on the other hand, tends to be stacked multiple holes with thick surrounding irregular scarring. It must be remembered, however, that many patients who smoke also have asbestos disease and thus, one can have a combination of both processes simultaneously. Sometimes curvilinear lines are seen paralleling the chest wall. These can represent areas of dependent gravitational atelectasis, if the patient is lying supine or may even represent distended lymphatics. By turning the patient prone, this gravitational dependency clears, or the lymphatics drain.Undercalling (Missing) Disease: AKA False Negatives
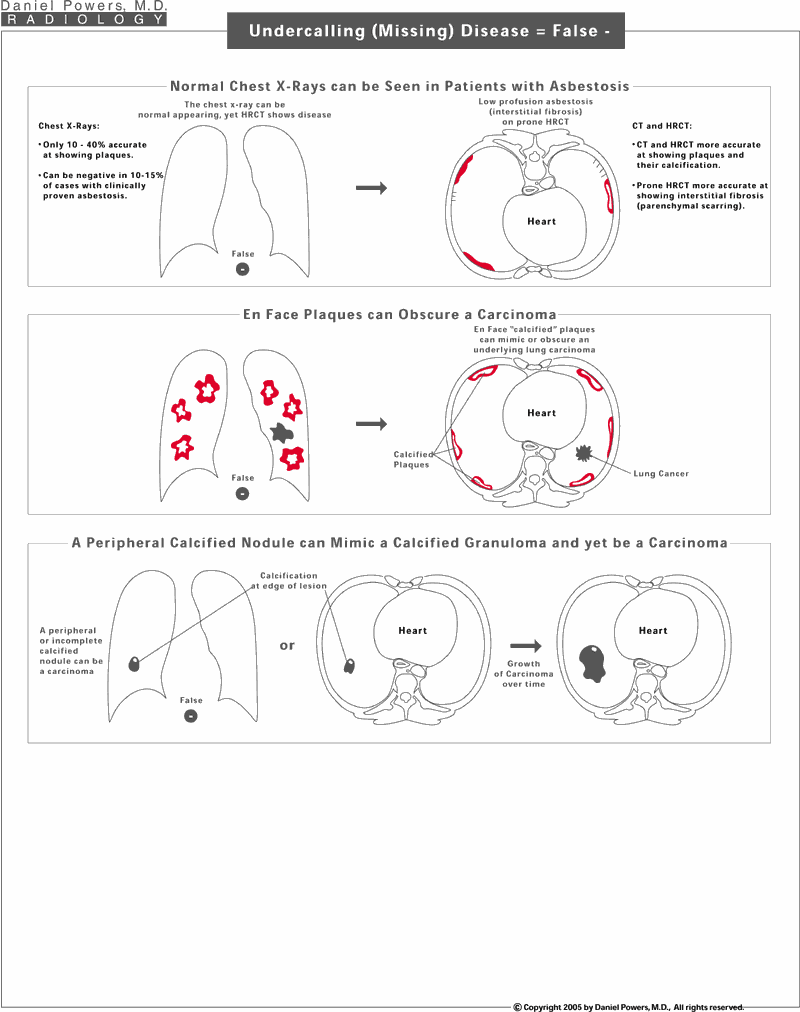
A normal chest x-ray can be apparent in an individual that truly has evidence for asbestos disease on CT or HRCT. CT and HRCT are more sensitive at picking up pleural plaques especially those with small calcifications, and individuals having low profusion (mild disease) may not have enough density on chest x-rays to visualize such a disease process whereas on prone HRCT, such findings are identified. It must be remembered that individuals with en face or face-on pleural plaques can also have a superimposed lung cancer. That is why it is very important to compare prior chest x-rays on individuals with such plaquing to the present x-rays to be certain that there are no new or changing densities or to obtain a follow-up supine spiral CT scan, which is able to separate out those densities along the chest wall from those that are in the lung. The mere presence of calcification associated with a nodule does not guarantee that is a benign scar or granuloma. If the calcium deposit is far on the periphery, this is often a warning sign that the nodule needs to be followed with sequential images to exclude growth since cancers can occur adjacent to a calcified area of tissue abnormality.Chest Findings Caused by Asbestos Exposure
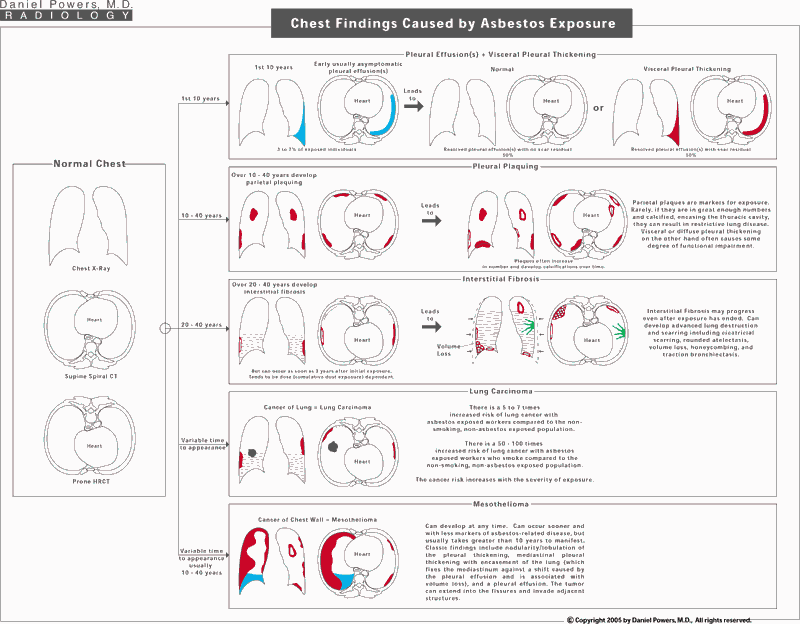
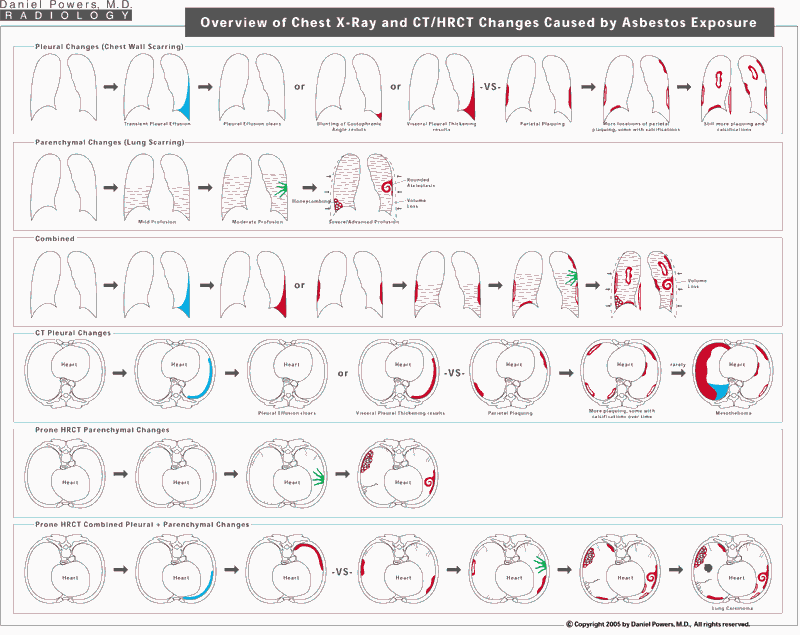
This represents a grand summary on single page of chest x-ray, supine spiral CT and prone HRCT findings associated with asbestos exposure.